|
4/23/2024 0 Comments Normal hip xray compared to oa The accuracy of intra-articular injection depends on the joint and on the skills of the practitioner and imaging may improve accuracy.According to current evidence, imaging features do not predict nonsurgical treatment response and imaging cannot be recommended for this purpose.Consideration of radiographic views is important for optimising detection of OA features in particular for the knee, weightbearing and patellofemoral views are recommended.To make additional diagnoses, soft tissues are best imaged by US or MRI and bone by CT or MRI. If imaging is needed, conventional (plain) radiography should be used before other modalities.However, imaging is recommended if there is unexpected rapid progression of symptoms or change in clinical characteristics to determine if this relates to OA severity or an additional diagnosis. Routine imaging in OA follow-up is not recommended.In atypical presentations, imaging is recommended to help confirm the diagnosis of OA and/or make alternative or additional diagnoses.Imaging is not required to make the diagnosis in patients with typical presentation of OA.The European League Against Rheumatism (EULAR) conducted a systematic review including 390 studies leading to seven recommendations concerning the use of imaging in peripheral joint OA as below: The study recommended that standard clinical algorithm for OA diagnosis, aided by radiographs is the most effective method for diagnosing OA. It concluded that MRI is more useful in excluding OA rather than diagnosing it. Important differential diagnoses include inflammatory arthritis (for example, rheumatoid arthritis), femoro-acetabular impingement, septic arthritis and malignancy (bone pain).Ī meta-analysis published in 2017 assessing the role of MRI in OA, assessed 16 studies which included 1220 patients. Suspected periarticular soft tissue pathology e.g. Suspected Osteonecrosis / Avascular necrosis of the hip.History of cancer or corresponding risk factors.History or family history of an inflammatory arthropathy.pyrexia, swollen and red joint, significant irritability, other risk factors of septic arthritis If imaging is necessary, the first-line investigation should be plain x-ray.Īn MRI or urgent onward referral may be warranted in some circumstances.  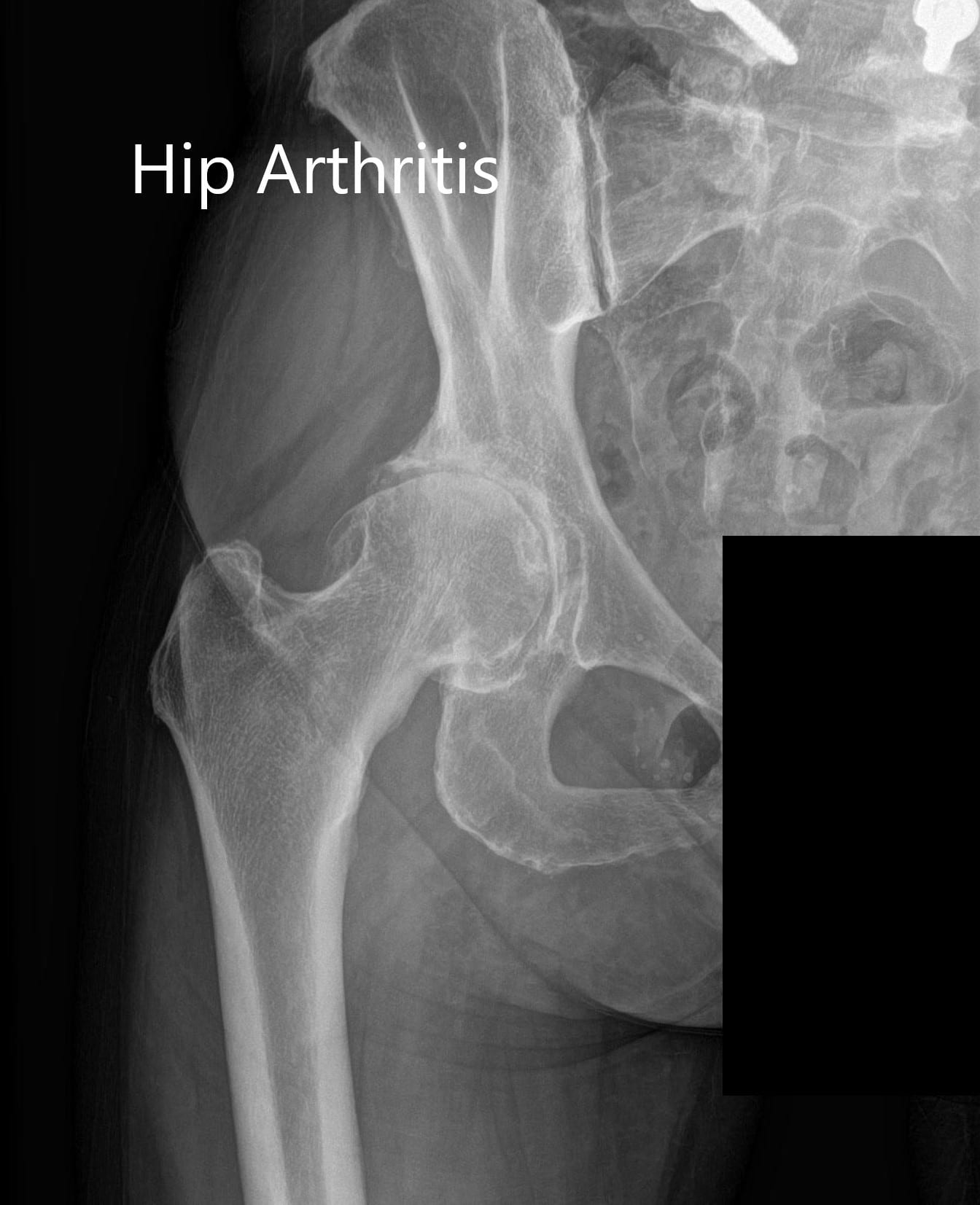
It is important to exclude other diagnoses, especially when red flags are present. Have either no morning joint-related stiffness or morning stiffness that lasts no longer than 30 minutes.NICE recommends diagnosing osteoarthritis clinically without investigations in patients who: The diagnosis of hip OA can be effectively made based upon the patient’s history and physical examination. Importantly it can cause unnecessary anxiety while waiting for specialist consultation and can delay MRI scans for patients with diagnoses other than OA of the hip. Requesting MRI scans further prolongs waiting times for patients. MRI scans rarely add useful information to guide diagnosis or treatment. Do not request a hip MRI when the clinical presentation (history and examination) and X-rays demonstrate typical features of OA. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
